These Screening Tests
Are For You
CONGRATULATIONS
You have decided to get screened. Now, which test is best for you? Ask your doctor – and here’s some basic information for that discussion.
There are three standard tests for CRC:
1. FOBTThe Fecal Occult Blood Test checks for blood in your feces. You take samples of your stools over three days, smearing the stool samples on a chemically treated card, and sending it to the lab for analysis. If blood is detected, you will be advised to have a colonoscopy. Pros and Cons: This is an inexpensive, widely available, do-it-yourself test, with no complicated prep. However, the FOBT is not fail-proof. Not all cancers bleed. It can detect some cancers but miss others. And some people find handling stool samples off-putting, so they put off doing the test. |
|
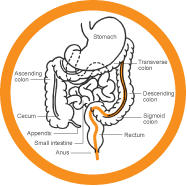
2. FLEX SIGThe flexible sigmoidoscopy is a finger-thin, flexible, lighted tube (the sigmoidoscope) with a tiny camera at its tip. The scope is inserted into your rectum, and up the bottom half of your colon – about 2 feet up (60 cm) – to check for polyps in the lower bowel: your rectum, sigmoid colon and your descending colon. Pros and Cons: The flex sig is a sensitive test for detecting polyps and cancer in the lower part of your colon. It rarely requires sedation and medical people other than doctors can be trained to administer it. The prep involves taking a mild laxative to empty your lower colon and you may be given an enema. This is a good test, but not perfect, because it misses about 35–40 per cent of polyps, the ones that are higher up in your colon.
Note: Many doctors believe that a yearly FOBT combined with a flex sig every five years is more effective in reducing colon cancer deaths than if you rely on just one of the tests. |
 CLICK TO ENLARGE IMAGE |
3. COLONOSCOPYA colonoscopy gives a whole new meaning to the phrase “Up Yours!” But it saves lives and allows the doctor to immediately remove any suspicious looking polyps that are found along the lining of your colon and rectum. The colonoscope is a thin, flexible tube with a camera at its tip, much like the flex sig, but longer. It lets the doctor examine the lining of your entire bowel and remove any polyps. If any are found, they will be sent to a lab and tested for cancerous cells. Frequently, the polyps are benign and with the colonoscopy “behind” you, those pesky polyps don’t get a chance to develop into cancer Pros and Cons: The colonoscopy is the only test that screens the entire colon AND allows immediate removal of suspicious polyps while you’re being examined. For those reasons, it’s often called the gold standard. But it’s not available everywhere, a highly trained physician must administer it, the prep is a bit daunting, and there is a very small risk – about 1 in 1,000 cases – of perforating the wall of the colon. |
 CLICK TO ENLARGE IMAGE |
What to REALLY expect with a colonoscopy
Preparation
This is, if you’ll excuse the expression, the shitty part of the procedure. You will be told to drink fluids the day before the colonoscopy, and empty your bowel completely. You’ll have to drink a few litres of water mixed with a laxative (your endoscopist will let you know which laxative to use and how much to drink). The mixture is easier to drink if you chill it; some people add a flavouring.
Plan to stay home, close to a toilet, while this process is underway. By the time you show up for the colonoscopy, your bowel will be clean as a whistle.
Note: Do not eat any seeds (this includes the tiny ones on raspberries and strawberries) in the week leading up to your colonoscopy. They can masquerade as polyps and cause all sorts of needless worry.
The Colonoscopy ItselfThis test should be painless. It’s performed in a doctor’s office or hospital clinic. You will be offered sedation. Go for it! It takes the edge off and helps you relax. The doctor will insert the scope up your anus, into your rectum and then carefully thread it through your entire colon. If you’re curious, you can watch it all on a video screen.
The doctor will examine your colon for polyps and snip off any that look suspicious. The entire scope usually takes less than half an hour. Some clinics encourage you to nap for a short time after the procedure. Arrange to have someone pick you up after the test. You shouldn’t drive after the sedation.
After the Test
If the doctor finds and removes any polyps, there may be a bit of bleeding. Let your doctor know if it persists. In the meantime, the polyps will be sent to a lab for review. Many are benign. If they turn out to be malignant, a specialist will “stage” the cancer and your physician will discuss treatment options with you.
Newer screening tests you may have heard about
The FIT
A variation on the FOBT, the fecal immunochemical test uses a more advanced laboratory method to detect the presence of blood in your stools.
The Virtual Colonoscopy
This test allows a radiologist to look for polyps without having to use a colonoscope. Advanced X-ray equipment is used to produce pictures of the colon and rectum. A computer then assembles the pictures into detailed images that can reveal the presence of polyps and other abnormalities. Because it is less invasive than a standard colonoscopy and sedation is not required, a virtual colonoscopy may cause less discomfort and can take less time to perform. The prep is the same – and if a polyp is found, you will then have to undergo a standard colonoscopy for polyp removal.
A CRC Blood Test
There are blood tests available that try to assess your current risk of having colorectal cancer, but they are not widely accepted by the medical community. The information the blood test offers can sometimes help determine whether you should have a colonoscopy. It does not diagnose the disease.
Stories that will get you off your butt – Bob's Story


 CLICK TO
CLICK TO